
Vesicoureteral Reflux
by
If your child has vesicoureteral reflux… urine is moving in the wrong direction, and has backed up from the bladder into the ureters and kidneys. The condition varies in severity, from mild or grade I, with urine backing up into the lower ureter, to severe or grade V, where urine back up into a swollen kidney.
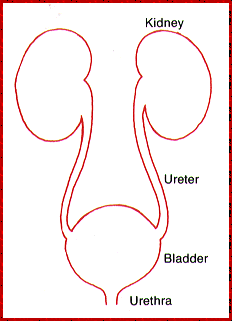
Urine is produced in the kidneys and normally flows into the ureters and bladder. Upon urination, it goes through the urethra and is eliminated from the body.
A valve mechanism located where the ureter enters the bladder prevents urine from backing up from the bladder into the ureters when the bladder empties. An abnormality in this valve may cause urine to flow back into the ureters. This abnormality is usually the result of a short length of ureter as it goes through the bladder.
Reflux is usually a congenital condition (children are born with it). Other less common causes of reflux include blockage to the bladder, abnormal urination with very high pressure within the bladder, dysfunctional voiding, or urinary tract infections.
Diagnosis requires an x-ray… examination called a voiding cystourethrogram (VCUG). A small tube is placed into the urethra and the bladder is filled with fluid visible on an x-ray. This study is done with your child awake and takes about 15 minutes. It is often combined with an ultrasound test of the kidneys.
Tests for reflux are usually recommended after a urinary tract infection… Reflux is comparatively common following urinary tract infections, occurring in about 40% of newborns and infants, and 25% of older children. It is very important to evaluate children with urinary infections for reflux, since the infection may be the only indication of the problem. The combination of reflux and infection can lead to kidney damage called reflux nephropathy which in turn can lead to kidney failure.
Treatment depends on the severity of the reflux… as well as the frequency of recurring urinary infections, and the ability of your child to take medication.
Usually children with grade I, II and sometimes grade III reflux can be treated without surgery. Your child will be kept on a continuous low dose of antibiotic until x-rays are repeated in one year. Medication by itself will not cure the reflux. Many children stop their reflux with age and growth, so the purpose of the medication is to prevent urinary infections and possible kidney damage during this time. Urine cultures must be obtained every six to eight weeks and at any time an infection is suspected. You should look for symptoms of burning with urination, frequency, abdominal pain or fever. An infection which develops while the child is on medication may be an indication for surgery.
Follow-up x-ray studies are then necessary to see if reflux has improved or been eliminated. Either a repeat of the VCUG or a radionuclear cystogram will be performed, as well as a renal ultrasound exam. At this point a decision can be made on continuing antibiotic treatment, or moving to surgical correction.
Surgery is recommended in some cases.. particularly those for more severe degrees of reflux, persistent reflux with fever, or repeated urinary tract infections. The operation is successful 95% of the time in correcting the condition.
Surgery involves creating an incision in the lower abdomen, opening the bladder, and reconnecting the ureter to the bladder to create an anti-reflux valve in the bladder wall. This operation can sometimes be done by going behind the bladder and creating a valve without opening the bladder. The operation takes about two hours and no artificial materials are used.
An experimental approach for correcting reflux involves injecting a Teflon paste into the bladder around the entrance of the ureter. This is an experimental procedure and its long term effects are unknown.
Treatment of reflux depends on many variables.
This discussion merely serves as an introduction to the condition of vesicoureteral reflux. I encourage you to personally discuss with me questions and concerns about your child’s treatment.
Return to the PedsUroLogic Home Page

Richard M. Parker, M.D., F.A.A.P., F.A.C.S.
[email protected]